Testicular Cancer
Testicular carcinoma is a rare type of cancer with only 2% abundance frequency in men. However, it is often in young men and boys of 15-34 years old, consistng the third more often type of death.
Most cases (i.e. 90%) of testicular carcinoma are due to stem cells alterations while only 10% due to testicular stroma.
Usually it appears as a painless contralateral thickening or nodule or as a hard mass in the testicle and concerns often right testicle, while 1-2% occurs bilaterally.
 Pathogenesis
Pathogenesis
It is virtually unknown. Occasionally, various risk factors have been implicated such as trauma, recurrent infections, estrogen administration to mother during pregnancy etc. Age, race and cryptorchidism are the only known risk factors, with the majority being found in men aged 20-40, children up to 10 years and masters over 60 years. The white race has 4 times more chances of developing these tumors while patients with a history of cryptorchidism have 3 -14 times greater likelihood of developing this tumor.
Most tumors of the testes derive from the stem cells of the testes and it’s most frequent types include seminoma and embryonic carcinoma.
The testicle usually shows a hard painless swelling that the patient usually finds himself. Rarely heaviness and pain or inflammation coexists. Reactive hydrocele may also coexist.
In many patients, especially when diagnosis is deayed; metastases’ symptoms appear such as flank pain, cough and dyspnea.
At diagnosis, laboratory tests play an important role. These, include:
Biochemical tests:
Beta-human chorionic gonadotropin (b-HCG),
A-fetoprotein (AFP),
Lactate dehydrogenase (LDH) and
Placental alkaline phosphatase (PLAP) which are characteristics high in certain cancers.
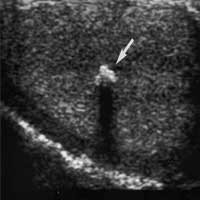
Scrotal ultrasonography: when testicular cancer is suspected, a scrotal ultrasound is immediately ran to investigate the suspicious area.
Chest radiograph and computed tomography are also used for the detection of metastases.
The final diagnosis is made after testicle excision (orchiectomy) and histological examination
 Pathogenesis
It is virtually unknown. Occasionally, various risk factors have been implicated such as trauma, recurrent infections, estrogen administration to mother during pregnancy etc. Age, race and cryptorchidism are the only known risk factors, with the majority being found in men aged 20-40, children up to 10 years and masters over 60 years. The white race has 4 times more chances of developing these tumors while patients with a history of cryptorchidism have 3 -14 times greater likelihood of developing this tumor.
Most tumors of the testes derive from the stem cells of the testes and it’s most frequent types include seminoma and embryonic carcinoma.
Pathogenesis
It is virtually unknown. Occasionally, various risk factors have been implicated such as trauma, recurrent infections, estrogen administration to mother during pregnancy etc. Age, race and cryptorchidism are the only known risk factors, with the majority being found in men aged 20-40, children up to 10 years and masters over 60 years. The white race has 4 times more chances of developing these tumors while patients with a history of cryptorchidism have 3 -14 times greater likelihood of developing this tumor.
Most tumors of the testes derive from the stem cells of the testes and it’s most frequent types include seminoma and embryonic carcinoma.

