This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
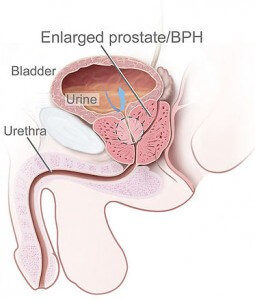
Benign Prostate Hyperplasia – general
About “prostate”
The term “prostate” was first used by Irofilo of Alexandria in 335 BC to describe the organ located in front of the bladder (foresail).prostatis
The “prostate” begins to form at the end of the 11th fetal week under the influence of androgenic stimulation of fetal testes and ends on the 16th fetal week. The gland development depends on dihydrotestosterone, estimated around the 4th month of gestation, the structure of the organ is complete.
Despite the fact that the old classification of prostate lobes is useful in daily practice, the understanding of the anatomy suggested by Mc Neal helps to further deepen the pathology of the organ.
The zones described by Mc Neal are:
- The transition zone [transition zone (TZ)]: represents 10.5% of the volume of the gland and consists of two lateral lobes. From this zone develops benign prostatic hyperplasia and 20-25% of prostate cancers.
- The central zone [central zone (CZ)]: is 25% of the prostate volume and contains ejaculatory resources. 5-10% of prostate cancers occur in this zone and a large percentage of inflammation.
- The peripheral zone [peripheral zone (PZ)]: is 70% of the volume of the instrument. In this anatomical region displayed the highest rate of prostate cancer (65-70%).
- The anterior zone (anterior zone): consists mostly of inomyika elements and contains no glands.
The prostate gland grows under the influence of multiple factors, the foremost of which are the androgens. Dominant role in this process plays testosterone (T).
The latter, by means of the enzyme 5-alpha reductase (5aR) is converted to dihydrotestosterone (DHT). In the adult, the synthesis of testosterone, a percentage of about 95%, is performed in the testes and more specifically by cells Leydig. The entire process is under the control of the hypothalamic-pituitary axis and in particular the levels of luteinizing hormone (LH). The remaining 5% of circulating testosterone is derived from the adrenal gland.

